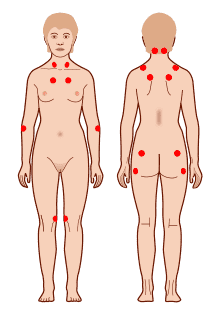
Fibromyalgia - treatment
Treatment focuses on relieving symptoms. Treatment of fibromyalgia depends on the symptoms, their type and severity, as well as the patient’s age and general health status.
Mild cases may improve significantly simply by reducing stress and improving lifestyle habits. Avoiding stressors is not always possible, which is why learning to self-regulate sympathetic nervous system activation – for example, using biofeedback – can be helpful.
More severe cases may require complex treatment delivered by a team of specialists. Depending on the symptoms, this may involve cooperation between a neurologist, rheumatologist, psychiatrist, psychologist, psychodietitian, and physiotherapist.
-
Pain-relieving medications (non-steroidal anti-inflammatory drugs) and sleep aids
-
Medications approved for the treatment of fibromyalgia (duloxetine, pregabalin, and milnacipran)
-
Antidepressants
-
Neurofeedback
-
Exercise and physiotherapy to stretch muscles and improve cardiovascular function
-
Massage
-
Heat therapy, cold therapy
-
Dietary changes: An anti-inflammatory diet, rich in antioxidants and fibre, may help alleviate fibromyalgia symptoms. Low-glycaemic index foods, such as selected vegetables or wholegrain products, help stabilise blood sugar levels, which may reduce inflammation and improve overall wellbeing. Balancing the intake of high-glycaemic index foods – which can lead to inflammation and fatigue – is also recommended. Many other factors are considered by a psychodietitian when developing a treatment plan.
-
Treatment of fibromyalgia with TMS (Transcranial Magnetic Stimulation)
Fibromyalgia is associated with central sensitisation — a state in which the nervous system becomes hypersensitive and overreacts to pain stimuli, even those that would not normally cause pain.
TMS (Transcranial Magnetic Stimulation) is a non-invasive and safe treatment method that uses magnetic pulses to precisely stimulate specific areas of the brain.
In fibromyalgia therapy, it focuses on modulating the activity of certain brain regions, which helps normalise pain perception and significantly reduce it.
As a result, patients often experience improved functioning and quality of life — often without the need for medication. -
mPNS in fibromyalgia therapy:
A modern and non-invasive method of pain treatment, based on Magnetic Peripheral Nerve Stimulation (mPNS), works similarly to the popular Transcutaneous Electrical Nerve Stimulation (TENS) — stimulating the peripheral nervous system.
However, unlike TENS, which uses electrical impulses, this technique uses magnetic pulses. This allows stimulation of deeper nerve structures without direct contact with the skin and without causing unpleasant sensations.
In fibromyalgia treatment, mPNS primarily works by modulating the peripheral nervous system, leading to reduced muscle tension and decreased transmission of pain signals to the central nervous system.
Although the effect of mPNS on central sensitisation is still being studied, there is evidence that peripheral stimulation may indirectly modulate central pain mechanisms, helping reduce chronic pain.
As a result, mPNS helps relax muscles, improve circulation, and support tissue regeneration, all of which contribute to an improved quality of life — without the side effects typical of pharmacotherapy.